Hemorrhoids — Symptoms, Treatment Options & When Surgery Is Needed
Hemorrhoids are swollen veins in the lower rectum or anus. They’re very common and often improve with lifestyle changes and medications. In persistent or advanced cases, minimally invasive procedures or surgery may be recommended to relieve pain, bleeding, and discomfort.
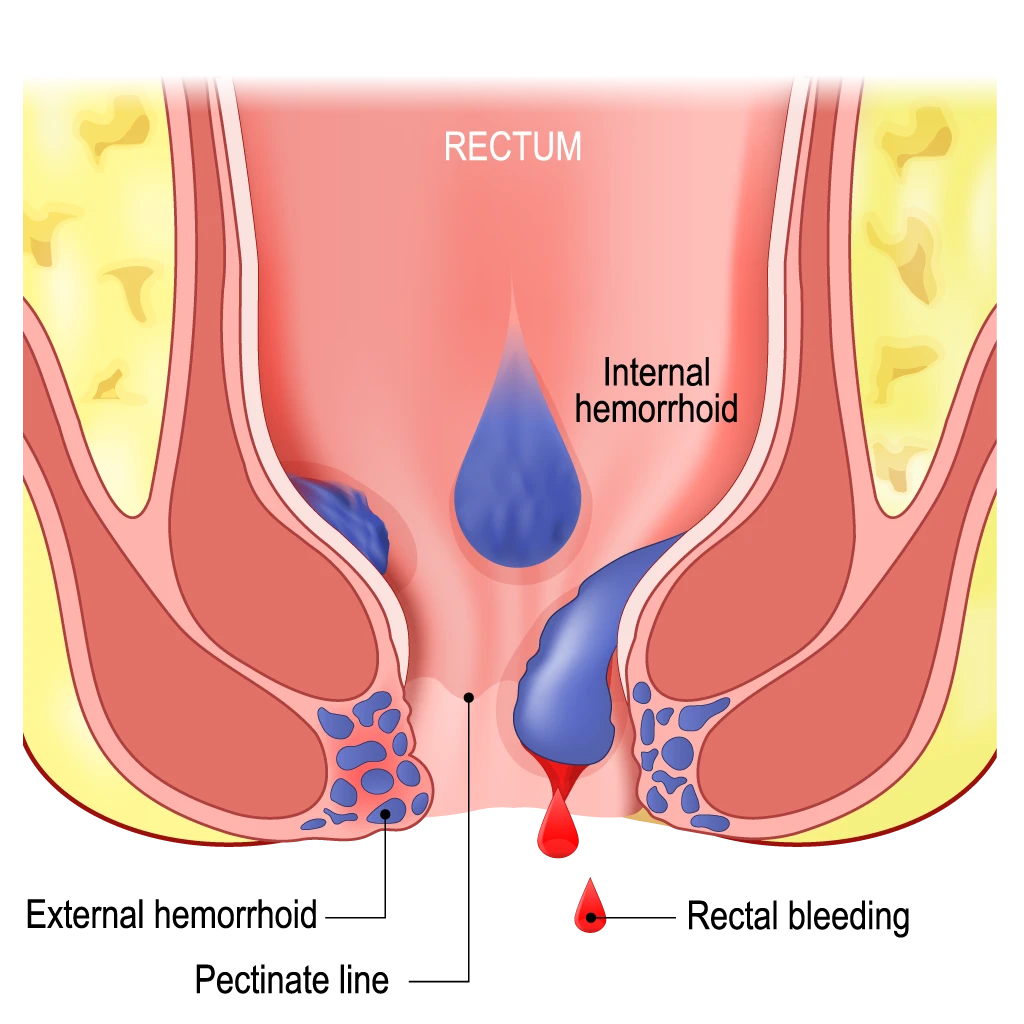
What Are Hemorrhoids?
Hemorrhoids can be:
- Internal (inside the rectum) — commonly cause painless bleeding
- External (under the skin around the anus) — can cause pain, swelling, itching
- Thrombosed hemorrhoids — a clot forms, causing sudden severe pain and a hard lump
Common causes include:
- Bright red blood with bowel movements
- Anal itching or irritation
- Pain or discomfort, especially with sitting
- Swelling or a lump around the anus
- Mucus discharge
- Prolapse (hemorrhoid protrudes outside)
Any rectal bleeding should be evaluated to rule out other causes.
Why Do Hemorrhoids Happen?
Common triggers include:
- Chronic constipation or diarrhea
- Straining during bowel movements
- Prolonged sitting on the toilet
- Low-fiber diet and dehydration
- Pregnancy
- Obesity
- Heavy lifting

Treatment Options
1) Conservative (First Line)
- High-fiber diet + fiber supplements
- More fluids
- Stool softeners if needed
- Warm sitz baths
- Topical creams/ointments (short-term use)
2) Office-Based Procedures (Minimally Invasive)
Used when symptoms persist:
- Rubber band ligation (common for internal hemorrhoids)
- Injection therapy (sclerotherapy)
- Infrared/thermal coagulation
3) Surgical Treatment (When Needed)
Recommended for advanced or recurrent cases:
- Hemorrhoidectomy (removal of hemorrhoids) — effective for severe hemorrhoids
- Stapled hemorrhoidopexy (for selected prolapsing internal hemorrhoids)
- THD / HAL-RAR (artery ligation techniques in selected cases)
The best option depends on the grade of hemorrhoids and your symptoms.
When Should You See a Doctor Urgently?
Seek evaluation if you have:
- Heavy bleeding or dizziness/fainting
- Severe pain and a hard lump (possible thrombosis)
- Fever or increasing redness/swelling
- Persistent bleeding, especially if over age 40 or with anemia/weight loss
Pre-Operative Evaluation (Typical Workup)
In the emergency setting, assessment may include:
- Physical exam and vital signs
- Blood tests (CBC, electrolytes, kidney function, inflammatory markers)
- CT scan (often the key test to locate the obstruction and detect complications)
- IV fluids and electrolyte correction
- Nasogastric (NG) tube for decompression if needed
- Antibiotics if perforation/ischemia is suspected
Recovery & Prevention Tips
Recovery depends on the cause and whether resection was needed:
- Avoid straining and prolonged toilet sitting
- Increase fiber gradually + hydrate daily
- Regular walking/activity
- Treat constipation early
- Maintain healthy weight

Why Choose Us?
With Dr. Ahmed Ali Abdelbary, your treatment is built around:
- Clear evaluation and procedure selection
- Patient-first safety approach
- Structured follow-up and guidance
- Modern bariatric and laparoscopic standards
FAQ ideas:
Some partial obstructions—especially due to adhesions—can improve with fluids and decompression, but surgery is required if there is complete blockage, worsening symptoms, or signs of complications.
Not always, but it can become an emergency quickly. Severe pain, fever, and inability to pass gas/stool are red flags.
Only in certain cases, depending on the bowel condition and safety of reconnection.
Book a Consultation
If you want a professional assessment and guidance on the most suitable option for your condition, book your consultation today.
